Psoriasis and Psoriatic Arthritis: Managing Skin and Joint Autoimmune Disease
 Apr, 6 2026
Apr, 6 2026
The Connection Between Skin and Joints
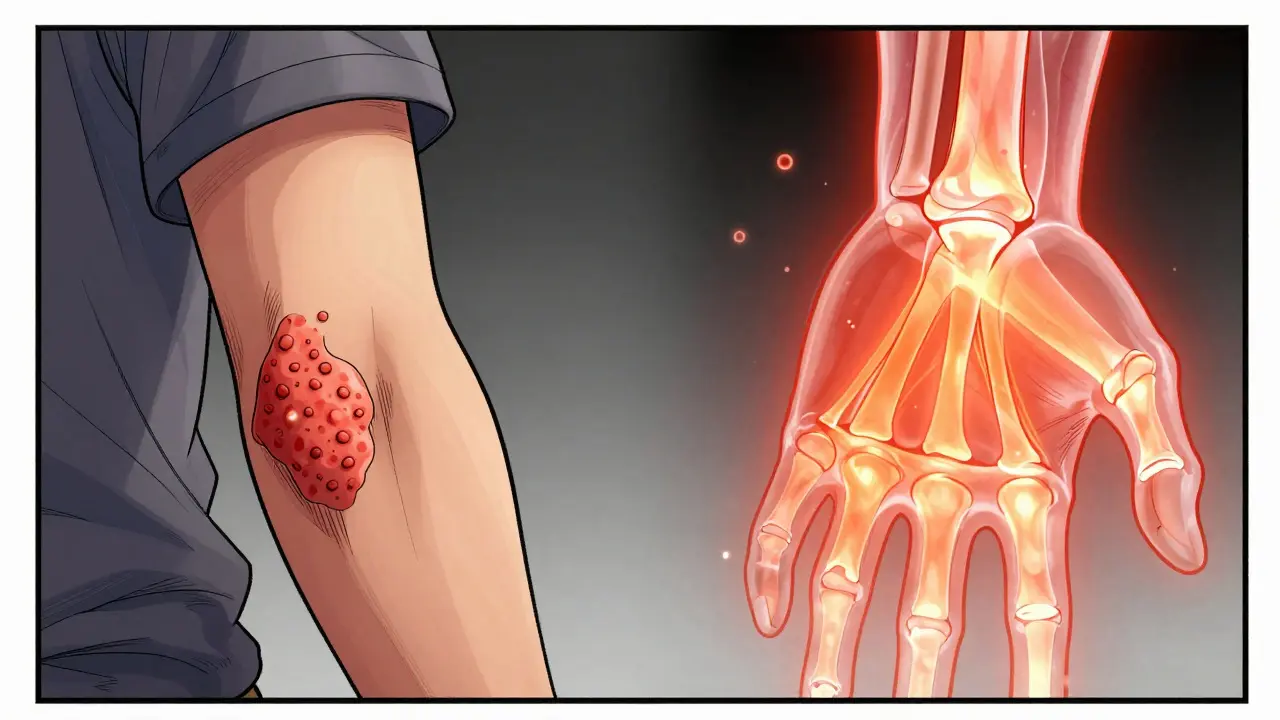
Most of the time, the skin shows up first. About 85% of people deal with psoriasis plaques-those red, scaly patches-long before they feel a tingle in their joints. However, it's not always that simple; in about 5% to 10% of cases, the joint pain actually appears before the skin rash. This suggests that the disease is systemic, meaning it's happening throughout the body, not just in one spot. When you have Psoriasis, your immune system speeds up the growth of skin cells. When that same overactive immune response hits the joints, it causes swelling and tissue destruction. If you've noticed pitting in your nails or they've started to separate from the nail bed, pay attention. About 80% of PsA patients have these nail changes, and they often serve as a warning sign that joint involvement is coming next.Spotting the Warning Signs: More Than Just Joint Pain
Joint pain is common, but PsA has some "signature" symptoms that help doctors tell it apart from rheumatoid arthritis or osteoarthritis. One of the most distinct is Dactylitis, often called "sausage digits." This is when an entire finger or toe swells up, not just one knuckle, making the digit look like a small sausage. This happens in roughly 40% of patients. Then there is Enthesitis. This is inflammation where your tendons and ligaments attach to the bone. If you have persistent pain in your Achilles tendon or the bottom of your heel (the plantar fascia), you might be experiencing this. It affects up to 50% of people with the condition and is a hallmark of the disease's preference for the edges of the joint rather than just the center.How Doctors Pinpoint the Diagnosis
Getting a diagnosis can be frustrating because the symptoms often wax and wane. To fix this, specialists use the CASPAR (Classification Criteria for Psoriatic Arthritis) system. Instead of relying on one blood test, they use a point system. You might get points for having current psoriasis, a history of the skin condition, or those characteristic nail changes. If your blood work shows a negative rheumatoid factor (which helps rule out other types of arthritis), that adds another point. If you hit a score of 3 or more, it's a strong confirmation of PsA. Beyond the point system, doctors often use imaging. X-rays can show a "pencil-in-cup" deformity, where the bone erodes in a way that looks like a pencil sitting in a cup. This is a late-stage sign, which is why early detection via MRI or ultrasound is becoming the gold standard to catch subclinical inflammation before the bone actually breaks down.| Feature | Psoriasis (Skin Focus) | Psoriatic Arthritis (Joint Focus) |
|---|---|---|
| Primary Symptom | Silvery, scaly plaques | Joint pain, stiffness, and swelling |
| Key Indicator | Body Surface Area (BSA) involvement | Dactylitis (Sausage digits) |
| Nail Changes | Occasional pitting | High prevalence (80%) of dystrophy |
| Systemic Impact | Localized skin inflammation | Enthesitis and possible bone erosion |

Treatment Strategies: From Pills to Biologics
Treatment isn't one-size-fits-all. The goal is to reach "minimal disease activity," which basically means you have almost no swollen joints and your skin is clear. For mild cases, NSAIDs (nonsteroidal anti-inflammatory drugs) can take the edge off the pain. If the disease persists, doctors often move to DMARDs (Disease-Modifying Antirheumatic Drugs) like methotrexate, which helps slow down the immune system's attack. When those aren't enough, Biologic Therapy comes into play. These are advanced medications that target specific proteins in the immune system. For example, TNF inhibitors (like adalimumab or etanercept) block a protein called tumor necrosis factor alpha, which is a major driver of inflammation. About 50-60% of patients see a significant improvement with these. If the skin is the biggest problem, IL-17 inhibitors (like secukinumab) are often more effective. Newer options like JAK inhibitors provide a different route by blocking signals inside the cells rather than on the surface.The Hidden Burden: Comorbidities
It's a mistake to think of PsA as just a skin and joint problem. Because it's a systemic inflammatory disease, the inflammation doesn't always stay in the joints; it can travel to the blood vessels and heart. Shockingly, about 40-50% of PsA patients have cardiovascular disease, and they face a 43% higher risk of heart attack compared to people without the condition. Metabolic syndrome-a mix of high blood pressure, high blood sugar, and abnormal cholesterol-is also incredibly common, affecting nearly half of all patients. On top of the physical toll, the mental strain is real. Dealing with a visible skin condition and chronic pain leads to depression and anxiety in 20-30% of cases. This is why a good treatment plan involves more than just a rheumatologist; it often requires a cardiologist and a therapist to ensure a high quality of life.
Looking Ahead: Precision Medicine
We are moving away from the "trial and error" method of prescribing meds. The next frontier is precision medicine. Researchers are now looking at the "gut-skin-joint axis," discovering that the bacteria in your gut microbiome might actually influence how your joints react to inflammation. New biomarkers, like serum levels of MMP-3, are being studied to predict which patient will respond best to a specific biologic before they even take the first dose. The target is to get the right drug to the right person within two years of diagnosis, potentially preventing the structural bone damage that used to be inevitable for many.Can psoriasis turn into psoriatic arthritis?
Yes. While not everyone with psoriasis will develop arthritis, about 30% of people do. It usually happens years after the skin symptoms appear, but it can happen simultaneously or even after joint pain starts.
What is the difference between PsA and Rheumatoid Arthritis?
The biggest differences are the presence of psoriasis skin plaques, nail changes, and dactylitis (sausage fingers), which are common in PsA but rare in RA. Additionally, PsA patients are typically negative for rheumatoid factor in blood tests.
Are there any permanent damages from PsA?
If left untreated, PsA can cause permanent bone erosion and joint deformity, such as the pencil-in-cup deformity. This is why early intervention with DMARDs or biologics is critical to preserve joint function.
Why do I have heart disease risk if I only have a skin condition?
Because psoriasis and PsA are systemic inflammatory diseases. The inflammation isn't just in your skin or joints; it can affect the lining of your blood vessels, increasing the risk of plaque buildup and heart attacks.
Can diet help manage psoriatic arthritis?
While diet alone cannot cure an autoimmune disease, managing metabolic syndrome through a heart-healthy diet (like the Mediterranean diet) can reduce overall inflammation and lower the risk of cardiovascular comorbidities.
